Root Canal Treatment
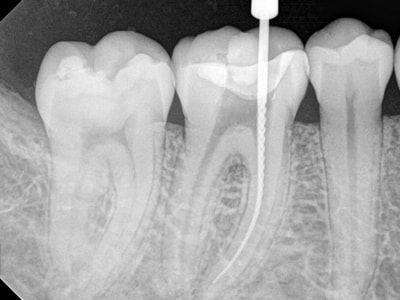
Root canal treatment is a procedure to maintain a tooth when the dental pulp has been damaged.
The pulp is the soft tissue within the tooth that contains nerves, blood vessels, and connective tissue. It extends from the crown of the tooth (chamber) to the tip of the root (root canals). The most common causes of damage to the pulp are tooth decay and tooth fracture (crack). Both of these problems can provide a pathway for germs (bacteria) to enter the pulp. When the pulp becomes infected, it can eventually die, leading to an abscess in the bone surrounding the root. When the infected pulp is not removed, pain and swelling can result. Without root canal treatment, the tooth will have to be removed.Steps in Root canal Therapy
The tooth will be examined, tested, and radiographs performed to determine if root canal treatment is necessary. During treatment, the dentist removes the diseased pulp, cleans the canals of the tooth, fills them, and seals the tooth. A local anesthetic will be given if necessary.
The following outlines the steps taken to maintain the tooth through root canal treatment. You may have to make more than one visit.
- To begin with, the dentist will administer local anaesthesia to make sure that you will not experience pain during the procedure.
- He will then isolate the tooth with a rubber dam, which is a thin sheet of latex rubber or plastic to keep the tooth dry and isolated.
- A cavity is prepared using a bur, in the crown of the tooth into the pulp chamber.
- The pulp or remaining tissue is then carefully removed from both the pulp chamber and the root canals.
- Each root canal is then cleaned and shaped to allow it to be filled.
- Medication may be placed in the pulp chamber and root canals to help eliminate bacteria.
- A temporary filling may be placed in the crown opening to prevent saliva from entering the chamber and root canals, or your dentist might immediately begin the next stage of filling the root canal.
- During the next stage of treatment, after placing the rubber dam, the dentist will remove the temporary filling (if one was placed during the previous visit). The root canals are usually filled with gutta-percha, a rubber-like material made from various tropical trees.
- In the final step, the temporary filling is removed and the tooth may be restored by a crown or a filling to strengthen and improve its appearance.
- The crown may be made of porcelain or metal alloy, and the filling may be made of many different materials.
- You might be prescribed antibiotics and other medication during the course of your treatment.
Believe in these before going for a root canal
Patients fear of root canal – It was believed to be one of the most painful procedure in dentistry and every patient who was advised to have root canal done used to fear to go to the dentist. But this is not a problem now, as good anesthetics are available which can subside the pain.
It is not time consuming – Earlier it used to take many visits for the completion of the root canal and this caused disturbance in the schedules of the patients and it was a hard task for them. Now it takes not more than 1 visit for the completion of the entire procedure.
Pain is not the only symptom- As said above, root canal should be done to prevent an infection, only the pain can not be taken as a factor to consider. If there is no pain in a particular region but there is some swelling with discoloration, the dentist have to properly check for the infection.
Better than extraction – It was believed entirely reverse of this. People used to believe in the fact that getting the tooth removed completely would be better than having root canal done. But maintaining the natural tooth for long can be helpful in proper chewing and strengthening of the tooth.
Also the cost for extraction is followed by its next procedure like removable denture or implant, which costs more than a root canal procedure.
Pregnant women – There are suitable anesthetics available for pregnant women and the x-ray required during the root canal treatment is small and focused only in the mouth region, so does not affect the abdominal region. So there is no restriction for pregnant women and they can have the root canal done, but prior to the treatment, the dentist should be kept aware about the fact that the patient is pregnant.
After Root Canal Treatment
There may be discomfort following root canal treatment. Over-the-counter medications such as acetaminophen, ibuprofen, or aspirin usually relieve discomfort. Dentist will prescribe or recommend medication for pain and/or infection if appropriate.If the pain lasts more than a few days, or if severe pain or swelling occurs, you should call your dental provider.
A permanent restoration (silver filling, composite filling, or crown) is critical to the success of root canal treatment because it helps to prevent bacterial contamination and tooth fracture.
Recall appointments. The root canal treatment, permanent filling, and/or crown are evaluated for healing at recall appointments every 6-12 months at no charge.
Good oral hygiene. Your restored tooth has a better prognosis if you commit to good oral hygiene and regular dental checkups and cleanings.
FAQs
First, an opening is made through the back of a front tooth or the crown of a molar or pre-molar.
After the diseased pulp is removed the pulp chamber and root canals are cleaned, enlarged and shaped in preparation for being filled.
If more than one visit is needed, a temporary filling is placed in the crown opening to protect the tooth between dental visits.
The temporary filling is removed and the pulp chamber and root canal permanently filled. A material called gutta-percha is inserted into each of the canals and is often sealed into place with cement.
In the final step, a crown is usually placed over the tooth to restore its natural shape and appearance. If the tooth is very broken down, a post may be required to build it up prior to placing a crown.How many appointments does root canal therapy take?
The number of visits it takes to complete your root canal treatment may be as few as one. With some cases, however, two or more scheduled appointments may be required.
The only alternative to a root canal procedure is having the tooth extracted and replaced with a bridge, implant, or removable partial denture to restore chewing function and prevent adjacent teeth from shifting.
If you, as a patient, have a preference or a need for short appointments (with the understanding that you will need to schedule more of them) you should let your dentist know.
Crowns
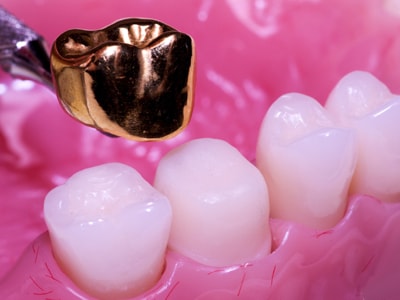
Dental Crowns
A dental crown is an ideal solution for dental patients who have one or more teeth that have enough healthy tooth structure remaining to support a prosthesis cap. A crown fits over the natural tooth and is bonded in place, providing a more even distribution of pressure across the tooth and root. It restores a tooth’s function and natural aesthetic appearance.Traditional crowns can cover teeth that have been partially damaged by chips, cracks, or decay. They protect the remaining healthy tooth. For patients who are missing a single tooth, a dental-implant supported crown is another option for restoration that fits over a dental implant titanium post. This is in contrast with a dental bridge, which affixes to natural teeth fitted with specialized crowns.
What are crowns made of?
There are three types of materials commonly used:- All-ceramic: due to the true revolution in dental industry. The “metal free” crowns are suitable for most cases. They combine excellent biocompatibility, high strength and high esthetics to ensure long-term success.
- Porcelain-fused-to-metal: the crown is made from both metal (precious or non-precious) and porcelain. PFM crown are still very commonly used for the back teeth but do not meet today’s esthetic standards for the front teeth.
- Gold: the use of gold crowns has significantly declined due to the importance of esthetic and the progress made in dental materials. However, in some cases they are still the best available option.
FAQs
Bridges
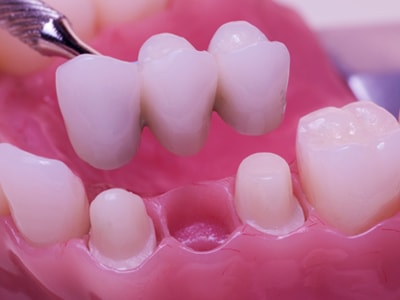
Dental Bridges
A dental bridge provides the same seamless appearance of a porcelain crown, crafted in our partner dental laboratory to match the color, shape, and size of remaining natural teeth. A bridge is a prosthesis comprising one or more artificial teeth that bridge a gap where teeth have been lost.
Using discreet attachments, the bridge prosthesis affixes to specialized crowns fitted over the natural teeth. Dental bridges have added stability because of their attachment to other teeth.
Our team of dental experts may recommend a crown to:
- Protect a weak tooth from breaking, or hold together segments of a cracked tooth
- Restore an already damaged tooth
- Replace a large filling when there is not enough tooth remaining
- Hold a dental bridge in place
- Cover a dental implant
- Cover a badly shaped or severely discolored tooth
- Cover a tooth that has had root canal treatment
Dentures
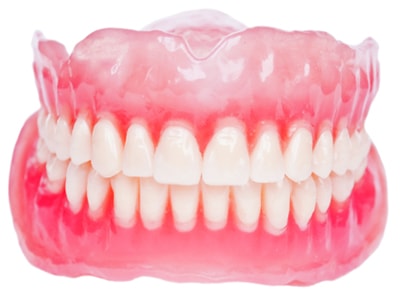
Full or partial tooth loss, if left untreated, doesn’t just affect a person’s self-image — it can also increase the risk of developing nutritional problems and other systemic health disorders. Fortunately, there’s a reliable and time-tested method for treating this condition: full or partial dentures. Dentures are the original false teeth. Partial dentures fill in the gaps where several teeth are missing, while complete dentures replace an entire set of teeth.
The fit of dentures is very important. They should fit well enough that they do not require the regular use of an adhesive. Top palette dentures often sit better in the mouth due to the suction that is created. Bottom dentures rarely fit 100%.
Unfortunately, dentures do not stop the bone less that comes with missing teeth—in fact, if you haven’t had teeth for many years, the bone loss is so great that a good fit is very difficult. And since the bone continues to deteriorate, you will need to be refitted for a new set of dentures every five to seven years.
Dentures are just one option for replacing missing teeth; some of the others include fixed bridgework and dental implants. Each method has its particular pluses and minuses, which should be carefully considered. There are also several varieties of dentures available to address specific issues, from partial dentures to implant-supported overdentures. During a consultation, we can explain the available options and help determine which is best in your individual situation.
How Do Removable Dentures Work?
Full or partial dentures consist of a gum-colored base made of plastic resin, which fits over the remaining alveolar (bone) ridge that formerly held the teeth. The prosthetic teeth projecting from the base are designed to look and function just like your natural teeth. Dentures are held in place primarily by the suctioning effect of their close fit against the alveolar ridges — that’s why it’s so important that they are fitted properly. The upper denture also gets extra support from the large surface area of the roof of the mouth (palate), which generally makes it extremely stable.At first, wearing dentures may require some getting used to in terms of talking and eating, as the dentures become “balanced” in the space formerly occupied by the teeth. But over time, the muscles, nerves and ligaments of the mouth learn to work in new ways, which allows these functions to occur normally. Dentures also help support the facial skeleton and the soft tissues of the lips and cheeks, which can help create a more youthful appearance. Immediate Dentures: These are usually a temporary means of helping you transition to successful denture wearing. Because of the muscular readjustment required, as well as the natural shrinkage of gums, the dentures which are placed immediately after tooth extraction won’t fit as well as permanent dentures made when the healing is complete. They do, however, provide you with new teeth right away, and give you time to adjust.
Conventional Full Dentures: After a period of time, we can fabricate permanent dentures that conform to your mouth with near-perfect accuracy. These are carefully crafted to look as much like your own natural teeth as possible, and are able to function properly in your mouth for a long time.
Implant-Supported Overdentures: To increase the stability of a lower or upper denture, it’s possible for it to be securely anchored using two or more dental implants. The upper jaw requires more implants (generally three or more) than the lower jaw due to a lesser bone density. Many people find this option offers a great balance of comfort, functionality and value.
Types of Partial Dentures
Transitional Partial Dentures: These relatively inexpensive removable plastic dentures serve as a temporary tooth replacement and space maintainer as you wait for your mouth to heal from tooth extraction, for example. Once the healing process is complete, dental implants can be placed.Removable Partial Dentures (RPDs): Usually made of cast vitallium, these well-constructed, metal-based removable partial dentures are much lighter and less obtrusive than those made of plastic. They are a little more expensive than plastic dentures but will fit better. They are, however, much less expensive than implants or fixed bridgework.
How Dentures Are Made and Fitted
Making quality dentures is a blend of science and art. First, an accurate impression (mold) is made of the alveolar ridges on the top and bottom of your mouth. The base of the denture is made from this mold in a dental laboratory. Working together, the dentist and lab technician choose from among many different sizes and shapes of prosthetic teeth to re-create a natural-looking smile. When everyone is satisfied with the result, the temporary dentures are made in permanent form.To enable normal speech and eating, it’s crucial to balance your bite. This means that the upper and lower dentures come together and properly stabilize each other. We carefully check the form and function of the dentures to ensure that they are working and fitting properly.
What to Expect After You Get Dentures
If you’ve recently lost your teeth and received an immediate denture, it’s normal to find some tissue shrinkage and bone loss occurring. Therefore, in several months you may find that your immediate dentures no longer fit well. You will have two choices at this point: You can have your immediate (temporary) dentures re-lined. This means that material is added under the denture’s base to better conform to the new contours of your alveolar ridge. A better option is to move to a set of conventional full dentures, which will last longer and fit better. With proper care, dentures offer a functional, aesthetic and economical solution to the problem of tooth loss.FAQs
If this irritation is left untreated, it can cause the gums and jaw to become inflamed and sore. You can get rid of the offending simply by removing and rinsing your denture. After a while your dentures should feel comfortable again.
Although your dentures are made to specifically fit your mouth, they may need to be adjusted over time due to changes which can occur in your mouth. In most cases these changes are perfectly natural and are normally due to aging.
It’s important to have your teeth evaluated by your dentist to determine if you’re a good candidate for bleaching. Occasionally, tetracycline and fluorosis stains are difficult to bleach and your dentist may offer other options, such as veneers or crowns to cover up such stains. Since teeth whitening only works on natural tooth enamel, it is also important to evaluate replacement of any old fillings, crowns, etc. before bleaching begins. Once the bleaching is done, your dentist can match the new restorations to the shade of the newly whitened teeth. Since teeth whitening is not permanent, a touch-up may be needed every several years to keep your smile looking bright.
If you’re not wearing your dentures they still need to be kept moist at all times, either by placing them in cold water or in a recommended denture solution to prevent them from drying out when not being worn. If you are suffering from problems you should contact your dental professional. They will be able to check your dentures and make any adjustments necessary. Never try to adjust your denture yourself, as this could result in permanent damage. Caring for your denture in the correct manner will give you years of trouble free service.
Toothbrushing – Brush your teeth at least twice a day (especially before going to bed at night) Brush at a 45 degree angle to the gums, gently using a small, circular motion, ensuring that youalways feel the bristles on the gums.
Brush the outer, inner, and biting surfaces of each tooth.
Use the tip of the brush head to clean the inside front teeth.
Brush your tongue to remove bacteria and freshen your breath.
Flossing – Daily flossing is the best way to clean between the teeth and under the gumline. Flossing not only helps clean these spaces, it disrupts plaque colonies from building up, preventing damage to the gums, teeth, and bone. Take 12-16 inches (30-40cm) of dental floss and wrap it around your middle fingers, leaving about 2 inches (5cm) of floss between the hands.
Using your thumbs and forefingers to guide the floss, gently insert the floss between teeth using a sawing motion.
Curve the floss into a “C” shape around each tooth and under the gumline. Gently move the floss up and down, cleaning the side of each tooth.
Inlays & Onlays
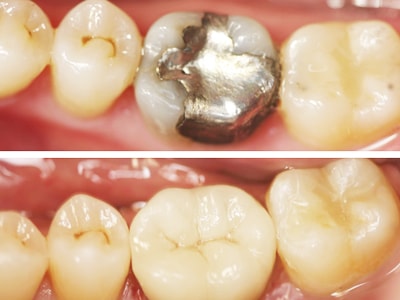
Dental inlays and onlays are restorations used to repair rear teeth with mild to moderate decay or cracked and fractured teeth that are not sufficiently damaged to need a crown.
Ideal candidates for inlay or onlay work typically have too much damage or decay in the tooth structure to be successfully treated using a filling, but have sufficient healthy tooth remaining to avoid the need for a crown. This allows the dentist to conserve more of the patient’s original tooth structure.
There are other benefits to inlays and onlays in comparison to metal fillings:
- Inlays and onlays are durable — they’re made from tough, hard-wearing materials which last up to many years.
- They help to strengthen teeth by up to 75 percent, unlike traditional metal fillings which can actually reduce the strength of the teeth by up to 50 percent.
- Inlays and onlays prolong tooth life and prevent the need for more dental treatment in the future.
During treatment the dentist removes the old fillings under local anesthesia and takes an impression of the tooth, which is sent to the dental laboratory. The new inlay or onlay is made from this mold in porcelain, gold or composite resin material. The inlay or onlay is then cemented into place at the next appointment. The inlay or onlay blends successfully with the treated tooth and the rest of the teeth to achieve a natural, uniform appearance.
How are inlays and onlays done?
It takes two appointments for the inlays and onlays treatment to be completed and to be finally bonded to the damaged area of the tooth.Inlays and onlays are performed using very similar procedures. At the first appointment, your dentist begins the procedure by numbing the area to be treated with local anesthetic. Any decay or damage is removed by drilling, which cleans and prepares the tooth for the dental inlay or onlay.
Using a small tray filled with dental putty that fits over the teeth, the dentist takes a mold (impression) of the damaged tooth. This impression is sent off to the dental laboratory, where a dental inlay or onlay is created that will fit your tooth exactly. Inlays and onlays are usually made from porcelain, which often most closely matches the normal color of the tooth, but they can also be made from composite resin or gold. While the inlay or onlay is being created at the lab, the dentist creates a temporary restoration (cover or filling) for your tooth to protect it until your next appointment.
At the second appointment, your dentist will remove the temporary restoration and then take time to ensure the inlay or onlay fits correctly. Only when the inlay or onlay fits perfectly will the dentist bond the inlay or onlay to the tooth with a strong resin adhesive. The inlay and onlay treatment is completed with a polish to ensure a smooth and aesthetically pleasing finish.
Each visit to the dentist for inlay or onlay treatment takes about an hour, with the first appointment taking slightly longer due to the preparation process. There will probably be a little discomfort after the inlay or onlay procedure, and the new tooth surface may feel a little odd, but you soon get used to the new tooth surface and how it feels and looks in your mouth. The tissue around the treated tooth may feel sore or sensitive, but this should subside in a couple of days. If you do feel some discomfort, you can take over-the-counter pain medication to alleviate the symptoms.